How Long COVID-19 Symptoms Differ Among Survivors
New Study Sheds Light on the Impact of Severe vs. Mild Illness
Published April 2023
If you have experienced long-term effects from a COVID-19 infection, often called long COVID-19, you likely have had — and may still be having — neurological symptoms such as dizziness, loss of smell or an altered sense of taste.
And, you aren’t alone.
“Long COVID occurs in approximately a third of COVID-19 survivors and is now the third-leading neurologic disorder in the United States, second only to tension-type headaches and migraine,” says Igor J. Koralnik, MD, chief of Neuro-infectious Diseases and Global Neurology at Northwestern Medicine and co-director of the Northwestern Medicine Comprehensive COVID-19 Center, overseeing the Neuro COVID-19 Clinic. “Long COVID has a significant detrimental effect in patients’ quality of life and has pushed an estimated 1 million people out of work in the U.S.”
Long COVID-19 is now the third-leading neurologic disorder in the United States.— Igor J. Koralnik, MD
While there isn’t a formal clinical definition of long COVID-19, it generally refers to symptoms lasting four weeks or more after infection.
Key neurologic symptoms of long COVID-19 include:
- Difficulty thinking, concentrating or memorizing (sometimes referred to as “brain fog”)
- Headaches
- Sleep problems
- Dizziness
- Pins-and-needles feeling
- Change in smell or taste
Symptom Differences
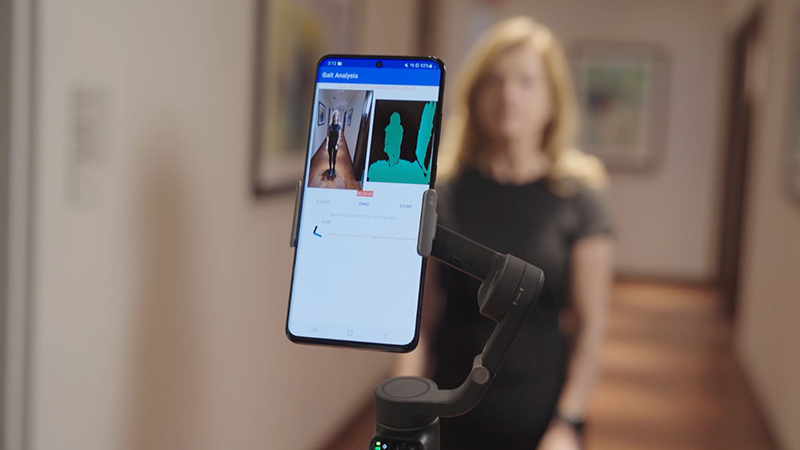
Scientists have discovered that long COVID-19 symptoms can differ depending on the severity of an initial COVID-19 infection. For example, if you had a severe infection, you may not be able taste food six months after hospitalization; your neighbor, who had a milder case of COVID-19, struggles to focus but can taste just fine.
In a recent study by Northwestern Medicine, scientists looked at data on the first 600 people with long COVID-19 evaluated at the Neuro COVID-19 Clinic. The study found that:
- People initially hospitalized for severe COVID-19 showed a broad pattern of cognitive impairment, ranging from brain fog to changes in smell and taste.
- People with milder illness who were not hospitalized mainly had difficulties with attention tasks.
Dr. Koralnik says patients who were hospitalized with COVID-19 could have widespread brain damage caused by a combination of low levels of oxygen in the blood, a severe immune reaction, the virus directly infecting the brain or multi-organ failure. These impacts may not be visible on brain imaging. “This is consistent with the broad cognitive dysfunction harbored by these patients,” he explains.
Personalized Care
Northwestern Medicine scientists plan to continue studying long COVID-19 to better understand its impact and how to personalize care for each patient.
People with neurological side effects of COVID-19 need specialized care to address the wide of range of possible symptoms. If you are experiencing neurologic symptoms after the onset of COVID-19 infection, talk to your physician.