Making Good On a Mission
When Northwestern Memorial Hospital Urology Chair Edward M. Schaeffer, MD, PhD, was training, the consensus at the time was that men with aggressive cancer couldn’t be cured. The best hope was to slow the cancer’s growth to extend the patient’s life. Unwilling to settle for such outcomes, Dr. Schaeffer made it his life’s mission to find a more effective treatment, with a cure as the ultimate goal.
The common understanding I encountered during training just wasn’t satisfactory to me. So, I made this work my life’s mission.
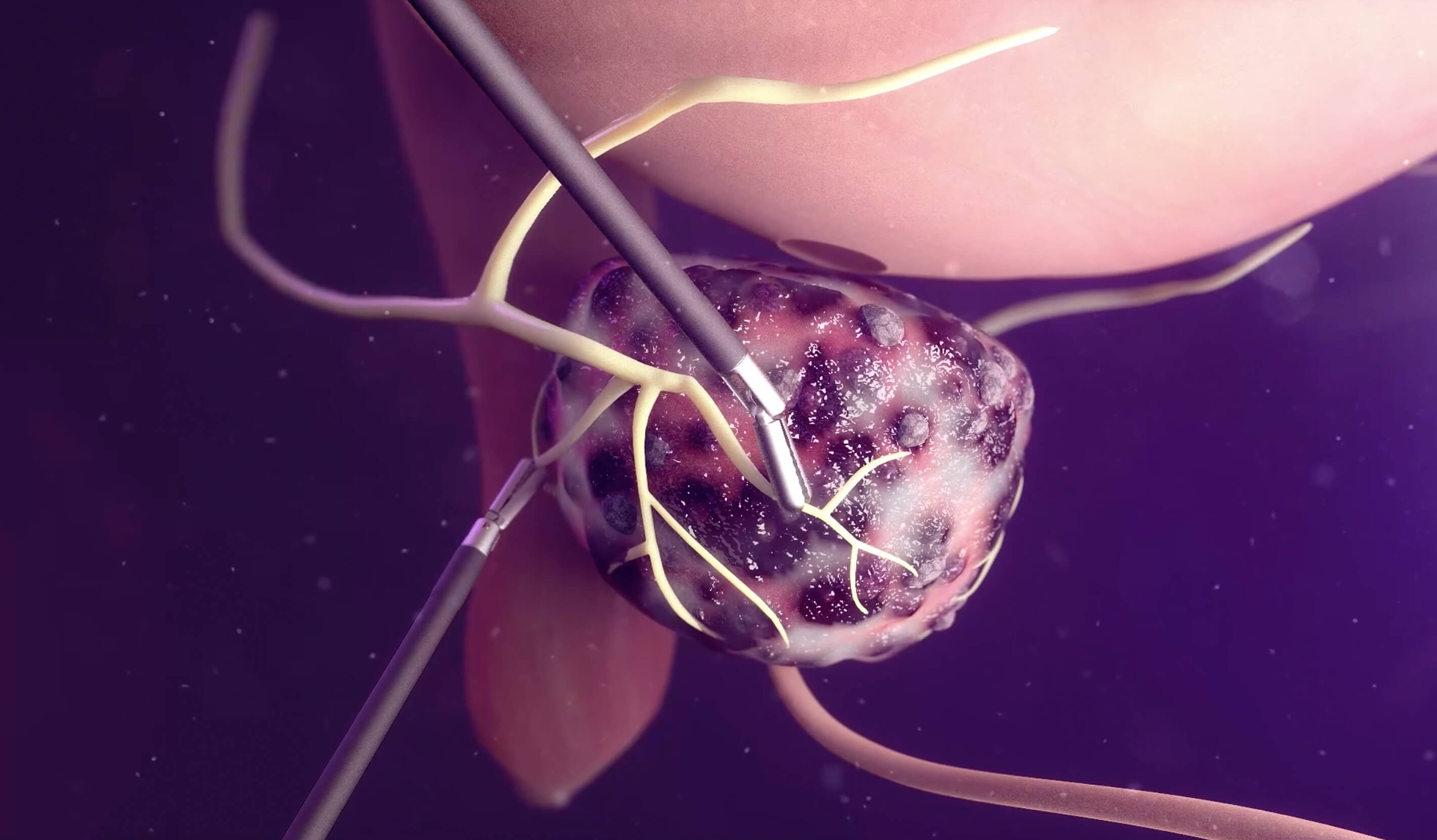
This made Dr. Schaeffer a perfect partner for Medical Oncologist Christopher M. George, MD, and the Radiation Oncology team at Northwestern Medicine Cancer Center Delnor. Working as a team with nationally ranked cancer program,* they were uniquely prepared to tackle Dave’s cancer. While Dr. George and the Oncology team would manage Dave’s traditional therapies, including hormonal therapy and radiation, Dr. Schaeffer would remove any cancerous masses through robotic surgery techniques. This specialized procedure was originally brought to Illinois by Dr. Schaeffer when he joined Northwestern Medicine, so he was perfectly suited to take on Dave’s case.
Dave was sent to me for simple, systemic treatment, and that’s that. But I asked Dr. Schaeffer to review his case, and together we soon realized that with a multimodal treatment plan combining surgery and radiation, we could offer Dave a real chance to live.
*Northwestern Memorial Hospital is ranked nationally by U.S. News & World Report, 2025–2026.







What makes us better, makes you better.®

WINNING THE RACE
A story like Dave’s is just one of many reasons why Northwestern Memorial Hospital, the anchor hospital for Northwestern Medicine, is the highest-ranked in Illinois for Urology.* At Northwestern Medicine, our collaboration, expertise and personalized teams are unparalleled. Today, Dave’s PSA level is normal, and there’s no trace of cancer in his system. He continues to see Dr. George and Dr. Schaeffer for regular checkups, keeping in touch with the world-class medical team that gave him a new lease on life.
I think we’re given a hell of a gift to be put on this earth, and you have to use it. Northwestern Medicine, and everybody involved, are the ones why I’m still here doing it.
Outcomes like these are why the teams at Northwestern Medicine take on the toughest conditions. At the age of 62, just one year after his surgery, Dave was back on his motocross bike and enjoying every second. It seems the only thing that’s changed for Dave is an upgrade to his bike: It now proudly displays a Northwestern Medicine decal.
*Northwestern Memorial Hospital is ranked No. 17 in the U.S. for Cancer and No. 10 for Urology by U.S. News & World Report, 2025–2026.