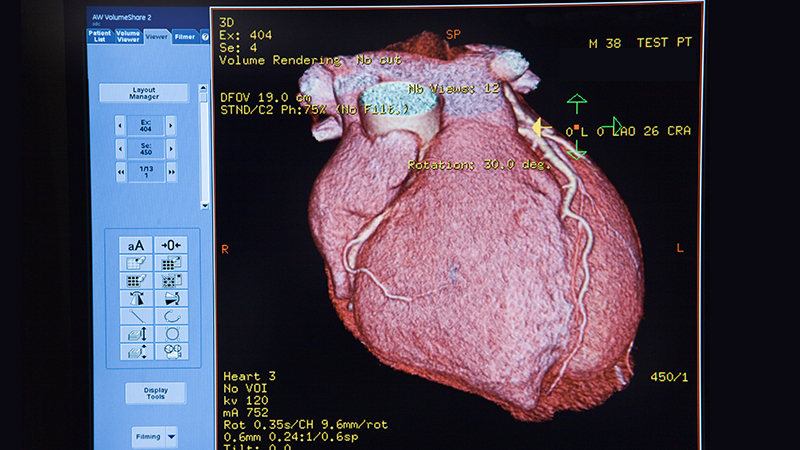
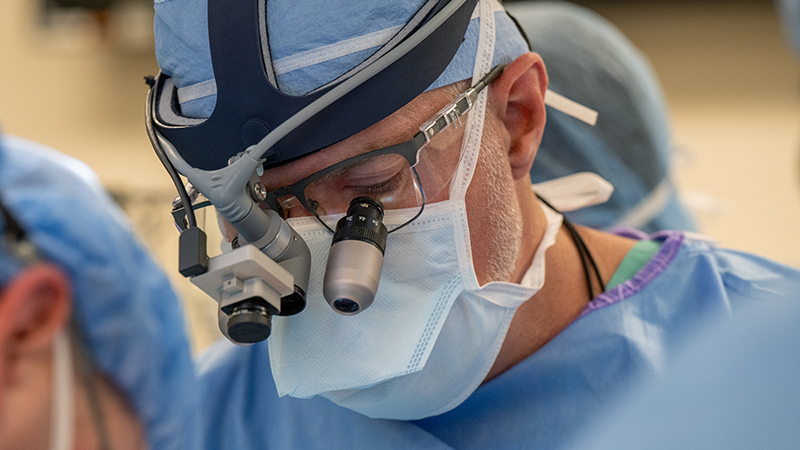
Your Journey to Better Heart Health
When you find out you have heart disease, you may feel overwhelmed and uncertain about the future. We understand, and we’re here to help.
At Bluhm Cardiovascular Institute, no one faces heart disease alone. We provide personalized, expert care to support you through every step of your heart health journey.

Take our risk assessment to learn more about your heart health.

Learn about your diagnosis and our expert care.

Recovery and Lifelong Management
We are your heart health partner for life.



 Our top heart specialists are ready to help you, no matter where you live. We know you want answers quickly, and through
Our top heart specialists are ready to help you, no matter where you live. We know you want answers quickly, and through